Do you experience sugar cravings after meals? Are you prone to becoming ‘hangry’ when you need to eat? These are very common things, but they may actually be a sign of insulin resistance- a common trigger for autoimmune diseases.
If you can remember from our previous blogs in this series, we use the acronym PTSD in functional medicine to assess areas of intervention when dealing with hormone imbalances. The “S” in that acronym stands for “sensitivity”, which refers to the level of sensitivity a cell has to a hormone. Insulin resistance is a prime example of how a cell’s sensitivity affects hormone levels. The cells become less sensitive to insulin, causing blood sugar to elevate in the bloodstream. Or, many times the hormone insulin becomes elevated significantly outside optimum ranges yet your glucose/A1c labs look normal! You may have all of the common symptoms but your doctor is not picking up on the precursor to elevated blood sugar, insulin levels >5. Have you had your fasting insulin tested recently?
What is insulin resistance?
Insulin is a hormone made in the pancreas by beta cells and its job is to regulate blood sugar levels. Beta cells also control the release of this hormone. When they are healthy, they will quickly create and release insulin in response to a spike in blood sugar after a meal.
Carbohydrates, fats, and proteins are broken down into glucose (sugar) molecules in your body. Your cells can use glucose for energy, but they need insulin to bind to their receptors in order for the glucose molecules to enter the cell.
When you consume a diet that is high in sugar and processed foods, your pancreas has to work much harder to control the blood sugar spikes associated. This can lead to either your pancreas not being able to keep up with the amount of insulin required, or the cells in your body that are constantly bombarded with insulin developing a resistance to it. Either way, more glucose (and inflammation) is left in your bloodstream. Here is a graphic illustrating this concept:
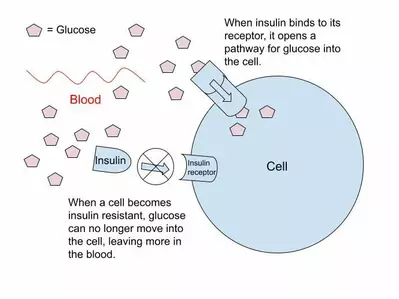
If insulin can’t help glucose enter cells and be used for energy, it will direct it to be stored as fat for later use (which can increase blood pressure, triglycerides and the hormone estrogen).. Insulin resistance is seen in many individuals who suffer from obesity (and you do not have to be obese to be insulin resistant).
When a cell is insulin resistant, its energy needs from glucose are not being met. Since the cells are essentially ‘starving’ for sugar, this can cause sugar cravings. High blood sugar and blood insulin levels can also trigger the body to store more fat. Higher fat levels in the body can lead to other complications by increasing inflammation. If insulin resistance and high blood sugar levels persist, prediabetes can occur and develop into Type 2 diabetes (or, Type 3 diabetes, AKA dementia).
Weight Loss Resistance
Insulin resistance is seen commonly in obese individuals as both an effect and a cause. Diabetes and obesity are huge issues in America. Over 40% of the US adult population suffers from obesity and nearly 45% suffer from prediabetes or Type 2 diabetes. According to the CDC, diabetes is the seventh leading cause of death in the United States!
Insulin resistance leads to more fat storage in the midsection/hips/breasts and leaves your cells starved for energy, resulting in sugary cravings. Weight loss can be very difficult for someone with insulin resistance for these reasons. If you’ve been struggling to lose weight, this could be an underlying cause.
Insulin Resistance and Dementia
Insulin resistance can result in brain cells not getting the energy they need, which may be why 80% of the diagnosed cases of dementia are directly connected to insulin resistance and people with diabetes are 50% more likely to develop Alzheimer’s. Alzheimer’s belongs to a class of dementias called ‘vascular dementias’, meaning it is caused by a blood-related issue and is likely reversible. You can drastically reduce your risk of developing dementia by getting insulin resistance or diabetes under control.
How does insulin resistance relate to PCOS?
Insulin resistance can be an underlying cause of Polycystic Ovarian Syndrome (PCOS). According to some studies, nearly 70% of women with PCOS also have insulin resistance.
High levels of blood insulin increase androgen levels (testosterone). Excess androgens in females are mostly to blame for the undesirable effects of PCOS, including acne, weight gain, facial hair, and weight loss resistance.
Beyond an ultrasound if you suspect PCOS you should be testing DHEA and fasting insulin levels!
What’s the solution?
Blood sugar levels can be regulated through diet and supplementation. Here’s a simple formula to keep in mind when you are putting together a meal: protein + fat + fiber (nutrient dense). Consistently getting these macronutrients will help your body naturally metabolize and balance blood sugar. Getting insulin resistance under control can in turn help reduce symptoms of PCOS related to excess androgens. Regular exercise is also a very effective and important tool for regulating your body’s insulin.
The most important aspect if IR is to find your root causes, remove them and track your results with objective lab tests. Don’t guess! Using standard labs and functional medicine will help track your progress and show you the results; but you surely will also feel it!
Here at Dr. Autoimmune, we offer a continuous blood sugar monitoring system so that you can find patterns in the foods that spike your blood sugar. This is one way we personalize a diet plan to fit your individual needs. We work with clients to find the root cause of their condition and develop a plan to help you reach your wellness goals. Contact us using the form below so we can get started!
Yours in health,
Ian Hollaman DC, MSc, IFMCP








